MERS – Viral Vector relevant bottlenecks
![]() Select parts of the map to find out more.
Select parts of the map to find out more.
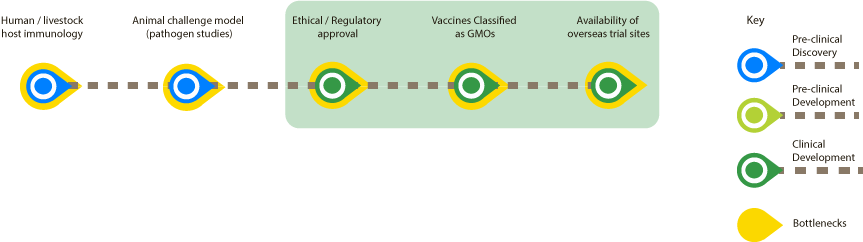
Please also visit Ethical and Regulatory Approval and the Use of vaccines classified as GMOs
Pre-clinical development – stages that areNOT bottlenecks due to the use of viral vector platform technology.
Masterseed bank production
From the research grade material it is necessary to go through a process of pre-GMP stock generation. This is done in the process development labs of our GMP manufacturing facility, following the principles of GMP, but without using a clean room. Some of this stock is then used to test the standard production process for replication-deficient adenoviral vaccines, some is used to test genetic stability and some will be taken into the clean room after appropriate QC testing in order to generate the master virus seed stock.
In general, this map does not apply to using platform technologies. Additionally our standard approach is to generate a master virus seed stock and small GMP batch for phase I testing within the same clean room campaign which also includes fill and finish, and proceed immediately to Phase I trials. No process validation is required for this scale of manufacture. Process development for scale up can occur in parallel with phase I and possibly phase II trials (first in human in the UK, further trials in other countries as appropriate). A small bridging study will then be required to compare the Phase I/II material with vaccine manufactured using the scaled up process.
The majority of assays required relate to the platform rather than the antigen. Antigen specific assays are used to test expression of the antigen (Western blot using serum developed in the pre-clinical stage) and to sequence the antigen in the viral vector (generic technique, antigen-specific primers required).
Antigen/vaccine identification
For this case study, a replication-deficient viral vectored vaccine expressing the major external antigen, the spike protein, is presented. This type of vaccine is safe to use in humans, can be manufactured at large scale and thermostabilised, is known to induce antibodies against the vaccine antigen in camels as well as humans, and also induce both CD4+ and CD8+ T cells against the vaccine antigen. The spike protein was chosen as it is the major external antigen of coronaviruses and infection can be blocked by neutralising antibodies to the receptor binding domain of this protein.
Pre-formulation work/in vitro, in vivo
No development work necessary as we are using a platform technology. A viral vectored vaccine (ChAdOx1) expressing MERS S was produced using standard techniques, tested for antigen expression by Western blot of the lysate from vaccine-infected cells, and then for induction of antibodies, neutralising antibodies (Marburg lab plus pseudotype neutralisation) and T cell responses after immunising mice. We were able to demonstrate high titre neutralising antibodies after one intramuscular dose of ChAdOx1 MERS, at the same level as that induced by two doses of MVA expressing the same antigen. Another group has shown partial protection of camels against MERS challenge after two doses of MVA (given by the intramuscular AND intranasal route at the same time).
Lead identification
Our lead candidate is ChAdOx1 MERS. Based on clinical development of other adenoviral vectored vaccines against Ebola virus it is expected that a single dose will induce high titre neutralising antibodies as well as CD4+ and CD8+ T cell responses in humans. There is also the option of boosting that response with a subsequent dose of MVA expressing the same antigen (this is being taken into clinical development by another group and we wish to collaborate once both vaccines are in clinical development).


